“Balance, standing tolerance, and joint stability are the tripod of mobility. Your must address all of them to improve one of them.”
Whether you have recently been hospitalized, had a bought of generalized weakness, a joint replacement surgery, chronic falls, or have a progressive disorder, balance is oftentimes the first thing to be affected. When your body has not been performing the right movements, your joints and muscles become weaker. As a result of this weakness, you may experience lower back pain when standing for more than 5 minutes, joint instability or “shaky knees and ankles”, and impaired balance creating a higher risk for falls.
What does a decline in balance, standing tolerance, and joint stability mean?
- You may have a muscle imbalance.
- Your visual perceptual skills may not be in sync with your brain-muscle communication.
- Your brain’s ability to communicate with your muscles, or certain muscles, and joints may have slowed down.
- You may be experiencing generalized weakness throughout your body and require a full-body ‘tune up’.
- Your body’s ability to understand where it is in space and adapt to various movements may be impaired.
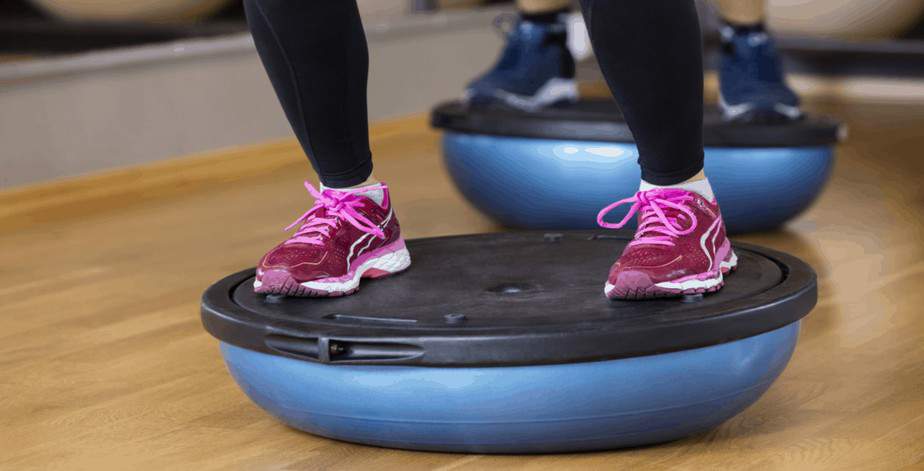
Muscles and Bones
Your rehab specialist is well-versed in upper body and lower body function. We understand how muscles and bones are designed to heal and can therefore use our vast knowledge of the human body and it’s systems to decrease muscle imbalances, help you become stronger and more flexible, and increase your upper and lower body joint stability.
Neurological Perspective
Neurocentric rehabilitation specialists understand the importance of starting at the source of movement and strength in order to yield the greatest and quickest results. We use many neurological-based therapy techniques such as neuromuscular re-education to increase your balance, standing tolerance, and joint stability.
Therapeutic Exercise and Therapeutic Activity
In our outpatient rehabilitation studio, we use many different techniques, strategies, tools, exercises and activities to increase balance, dynamic standing, and joint stability. Some tools and equipment we use are agility ladders, aerobic steppers, tandem walking surfaces, free weights, theraband, bosu balls, manual therapy, modalities, and much more! Doesn’t sound like occupational therapy? Read more about our hybrid approach to outpatient rehabilitation!
‘Real-Life’ Activities or Occupation-based Interventions
Occupation-based interventions are the most functional-based approach to rehabilitation. When you are invested in the activity and understand why you are doing something, your brain’s ability to heal and re-learn motor patterns improves exponentially! Occupational therapists are functional rehabilitation specialists which means we are experts in translating physical strategies into functional activities! We understand that performing a sit-to-stand in the studio is much different than getting up from your favorite recliner chair! Likewise, re-learning how to move your arm or walk in the studio is much different than feeling confident entering your home or moving about the community! Buffalo Occupational Therapy always bridges this gap and includes these real-life elements as part of our outpatient rehabilitation process!
- Ensure you are given a comprehensive evaluation by your therapist! It should include objective assessments, a work-up of upper and lower body strength and range of motion, a screen for reaction time and coordination, a cognition screen to ensure your memory has not been affected by decreased mobility, and a conversation or perceptual screen regarding your fear associated with falling.
- Commit yourself to at least 6 weeks of outpatient therapy after discussing the plan with your therapist. Improvement takes time! You can’t improve without commitment to a plan.
- Follow the Home Exercises Program (HEP) given by your therapist which will include exercises and stretches to promote balance, standing tolerance, and joint stability!
- If you live alone and have not had your house assessed, a home assessment is highly recommended. In this home assessment, a therapy practitioner will walk through your home and recommend way to increase safety, accessibility, and decrease potential fallings risks. A home assessment also allows the therapy practitioner to give you information of various pieces of adaptive equipment and durable medical equipment that may increase the liveability of your physical environment!
Are you facing a specific diagnosis or condition effecting your functional performance?
Check out some examples of conditions we treat through outpatient rehabilitation!
Why choose Buffalo Occupational Therapy?
Buffalo Occupational Therapy works with you one-on-one to create a treatment plan that will meet your needs, accomplish your desired outcomes, and restore your hope in recovery.
Buffalo Occupational Therapy practitioners are committed to maintaining current competencies, meeting monthly continuing education goals, and being well-versed in the latest evidence-based, research-driven treatment models in order to offer you the best treatment possible.
Specialized occupational therapy practitioners are accessible to their patients, invested in producing treatment plans that will produce results, maximize time spent, and offer you hope for recovery.
Buffalo Occupational Therapy is currently the first and only Neuro-centered adult outpatient occupational therapy practice specializing in neurological rehabilitation, functional performance, and rehabilitation for older adults.
Helpful Page Definititions
Muscle Imbalance
Your body is complex and should be working synergistically with all of its parts. When some muscles have become weaker while others remain strong, an imbalance occurs which causes decrease balance, standing tolerance, and joint stability.
Visual Perception
We incorporate visual perceptual elements into many treatments to enhance perception, balance, safety, cognition, memory, recall and neural excitation. Some areas of visual perception include form constancy, visual discrimination, figure-ground perception, visual closure, visual memory, and visual sequential memory.
Neuromuscular Re-education
NMRE is used by neurocentric occupational therapists to improve communication between your muscular system and nervous system. By promoting this stream of communication, you close the circle of recovery. Without NMRE, you can have the biggest muscles in the world and still experience mobility deficits due to poor reaction time, coordination, and mixed signals.
Comprehensive Evaluation
Occupational therapists treat the entire person. Much like your primary care physician, we were required to learn elements of the entire body so that we could treat holistically (a one stop shop). Because of this, your outpatient rehabilitation specialist will perform an evaluation that assesses the following things:
- Personal history
- Who are you? What do you do? What makes you tick? Why are you seeking outpatient therapy?
- Physical function (upper body and lower body)
- Strength, range of motion, and flexibility
- Neuromuscular function (brain to muscle communication)
- Coordination, speed, agility, and reaction time
- Cognitive and Mind health
- Short term memory, recall, information processing, and perception of illness
- Occupational Inventory (Activity and role inventory)
- Roles you play like a caregiver, spouse, parent, employee, etc.
- Mobility inventory like the places you need to go
- IADL inventory and what activities are required for you to be independent
- Other activities that are important to you
